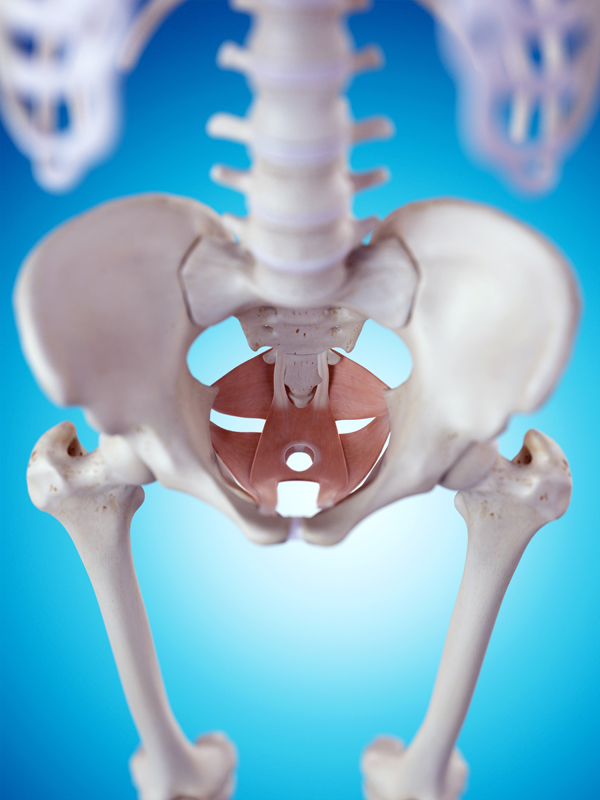
Pelvic floor strengthening and stretching – my story
/This blog talks about the different types of incontinence, one common after childbirth, one a possible hindrance to childbirth, how to strengthen your pelvic floor and how Women's Health Physiotherapists can help treat the complex issues.
We are comfortable talking about gay marriage and even sex toys, but incontinence is still taboo. It is actually very common but shouldn’t be. Understandably it is prevalent after vaginal birth due to the stretching of the pelvic floor more than one cares to imagine. It is also more prevalent during pregnancy too due to the pressure your growing baby is placing on your bladder and pelvic floor.
At 36 weeks the frequency to go to the toilet is increased in 81% of pregnant women, urge incontinence is present in 68% of pregnant women, stress urinary incontinence is present in 42% and bladder prolapse is seen in 14% of pregnant women (Van Brummen et al, 2006).
Six months after birth, 26% of postpartum women have sexual problems, 25% have haemorrhoids, and 10% have urinary incontinence (Brown and Lumley, 1998). So what is the pelvic floor exactly and what can we do to strengthen or stretch it?
“Urge incontinence is present in 68% of pregnant women, stress incontinence in 42%...”
The pelvic floor is made up of muscles and fascia that run from the pubic bone around the urethra (wee hole), vagina and anus (poo hole) and attach to the coccyx and tissues to the side.
As the name suggests they run along the floor (bottom) of the pelvis. There are two main layers of muscle with the deeper level containing the levator ani and coccygeus (the main pelvic floor muscles). The superficial muscle layer contains the external anal sphincter and urogenital triangle (3 muscles).
The pelvic floor muscles control the anal and urethral sphincters for continence but (along with the fascia) also support the pelvic organs including the bladder, intestines, uterus and rectum.
It also helps guide the baby to rotate forwards during birth.
If the pelvic floor is too weak bladder, uterus, rectum and intestine prolapse and resultant pessaries (fitted by specially trained physiotherapists) or surgery can occur.
A deep aching pain in your pelvic floor area is a symptom you will feel and suggests it is time to go and see your Women’s Health Physiotherapist or Doctor for management. I will talk about prolapse in more detail in Bladder, Uterus or Rectum Prolapse and Physiotherapy Management.
I am a very honest person but still find it hard to admit (especially in this very public forum!) that I have continence issues. I drink excessive amounts of water, my physiotherapist told me too much and I have a pelvic floor that is actually too tight and an overactive bladder.
An overactive bladder is when the detrusor muscle that contracts the bladder to empty it, goes in to involuntary spasm sometimes and can give me urinary urgency and sometimes incontinence.
Urgency is when you are close to home or hear water running and then you suddenly are busting to go and if you leak before you make it to the toilet that is Urge incontinence.
In part I blame my mother and grandmother who both suffered from it. It can be hereditary but encouraged by the habits you make to prevent incontinence accidents. Urgency is a very complex issue with many contributors but one cause of urge incontinence is going to the toilet “just in case” before you go on a trip.
This urge is due to a spinal reflex which you can learn to override. Physiotherapists can teach you some techniques to buy you time to get to the toilet and some permanent fixes.
The other form of incontinence is Stress incontinence is “the involuntary loss of urine on effort or physical exertion, or on sneezing or coughing” (Haylen et al, 2010- International Continence Society).
Stress incontinence is due to the urethral sphincter incompetence (pelvic floor weakness, a poorly coordinated pelvic floor, fascial damage, or loss of urethral sphincter muscle fibres).
Another cause of stress incontinence can be breastfeeding (or menopause) as in this time oestrogen is decreased which lower the urethral pressure which contracts the urethra to prevent incontinence. Stress incontinence is the form of incontinence that can result after vaginal child birth and something that you can also overcome with physiotherapy.
Anyway over the years I have tightened my pelvic floor ineffectively to try and deal with the urge incontinence. This tightness is not neccessarily a strong pelvic floor, just ineffective muscle tension. This tightness can also result as scar tissue from childbirth. So I have had to work on strengthening as well as stretching my pelvic floor. Only a physiotherapist who is trained in pelvic floor assessment will be able to tell you this and help you to rectify it.
It is highly recommended to have your pelvic floor tested when you are pregnant (preferably before) so that you can strengthen or stretch your pelvic floor appropriately to prevent incontinence, perineal tears (often if the pelvic floor is tight) which commonly leads to prolapse and long term issues. I was worried about perineal tears and increased pain with child birth as well as increased incontinence so was diligent in treatment with a physiotherapist.
The physiotherapist introduced me to this amazing product (of which I am not being paid to endorse). The EPI NO. It was useful for me early in pregnancy, at the end and postnatally. Money extremely well spent. This inflatable balloon is carefully inserted in to the vagina and then you can practice pelvic floor strengthening by getting biofeedback on the gauge seeing the pressure increase as you contract your pelvic floor muscles.
It is often hard to know whether you are contracting your pelvic floor muscles or not (without the guidance of your physiotherapist) but biofeedback machines can really help. To prevent any risk of miscarriage it is important to minimally inflate the balloon during the majority of pregnancy (especially in the first trimester).
I preface these instructions to say that 50% of women perform pelvic floor contractions incorrectly if only given verbal instruction so it is really essential to go and see a Women's Health Physiotherapist to check your contractions. But if you want to make a start on contracting your pelvic floor muscles, you need to think about where they are and then contract them from front to back or back to front, tightening and lifting the muscles surrounding your urethra, vagina and anus.
“stop the flow of urine or releasing gas or tightening your vagina for increased sexual pleasure...”
I always say to my patients, think that you are trying to stop the flow of urine or releasing gas or tightening your vagina for increased sexual pleasure.
It is important to not contract the bottom muscles because these are not going to help strengthen your pelvic floor or continence. If you put your finger underneath your coccyx (tail bone) and contract your pelvic floor correctly, your coccyx should move forward towards your vagina. This is why a physiotherapist is very helpful in guiding you through this.
It is important to do quick strong contractions so that you are not incontinent with fast activities like sneezing and jumping but also do longer 10 second plus contractions so that you can hold on when you are not near a toilet. We should practice these exercises multiple times per day for the rest of our lives. Like any muscle if we stop exercising it, it will become weak. Associate the exercise with something you do daily like brushing your teeth or having a shower.
After 36 weeks, the EPI NO can be used for my other problem, pelvic floor tightness. However, it is useful for anyone having a vaginal birth as through inflating the balloon gradually up to a 10cm diameter you can stretch the vagina and perineum to help prevent perineal tears and episiotomies. This then prevents incontinence as a result of preventing these tears/ episiotomies.
I also found it extremely helpful psychologically knowing if I could stretch my vagina to 10 cm and then push the balloon out without too much discomfort then child birth would not be that bad. Because stress increases pain, if I could decrease my stress this would also decrease the pain of childbirth. In the end, I ended up having a caesarean section so avoided all of these issues but I was so grateful to have this knowledge and preparation.
For those of you that have a natural birth (the vast majority), the pelvic floor is stretched and often torn or cut. If torn or cut scar tissue will result. The scar tissue leads to tightness and inflexibility and quite often pain in the tissues of the vagina, pelvic floor and sometimes rectum and can also be the cause of back pain.
“If pelvic floor is stretched or torn... leads quite often to pain with intercourse, pain with bowel motions, haemorrhoids and prolapse...”
Sexual problems such as pain with intercourse can result. Likewise, haemorrhoids or pain with bowel motions can result. Prolapse can occur due to the weakness, tears or avulsions (muscle detaching from the bone) of the pelvic floor that has not strengthened after childbirth.
If there is scar tissue this can make the pelvic floor harder to activate and more assistance may be required to learn how to activate the muscles. Scar tissue should be treated by a Women’s Health Physiotherapist with massage and stretches to prevent long term issues. Treatment of the pelvic floor may also fix back pain that has been caused by a referral of pain from pelvic floor issues.
Just an additional note, if you have/had a vaginal birth it is important to protect your pelvic floor as it recovers from being stretched, torn or cut. Doing gentle pelvic floor exercises as described above can be commenced in the first day or two post birth. As well as regaining strength and prevent stress incontinence, it can help reduce swelling and helps the healing process of scar tissue.
To avoid putting stress on the pelvic floor in the days after birth, go to the toilet as soon as you feel the need to go, when you empty your bowels put toilet paper up against your pelvic floor (in front of your anus) so you don’t overstretch the pelvic floor when your bear down. Also avoid strenuous activities or lifting anything heavy, drink plenty of water and avoid caffeinated or acidic drinks to prevent constipation and lastly when you cough or laugh tighten your pelvic floor muscles to help prevent stress incontinence.
One more thing; sensation to void is reduced just after birth and you have a lot of excess fluid to void so it is important to go regularly (not just when you feel the urge) to avoid severe expansion of your bladder which can cause very bad and long term damage to your bladder.
I hope through telling you my personal story you will feel comfortable asking me any of your questions about the pelvic floor and we can work together to get a strong flexible pelvic floor ready for pregnancy, child birth and beyond. If you feel comfortable you can share your story below to help ease the stigma of incontinence, a common but preventable problem.
Summary
Stress incontinence is common after vaginal delivery and occurs when you laugh, sneeze jump or run. This can be assessed and treated by a Women's Health Physiotherapist.
Urge incontinence occurs because your bladder muscle goes in to spasm. This commonly coincides with tight pelvic floor muscles which may need stretching by a Women's Health Physiotherapist to make childbirth easier.
Scar tissue from perineal tears and nerve damage from childbirth can make it hard to activate your pelvic floor and may need to be massaged/ stretched to allow pelvic floor activation. Women's Health Physiotherapists can help you with this.
Melli Tilbrook is a Physiotherapist based at Adelaide Physiotherapy and Pilates Studio, Beulah Park.