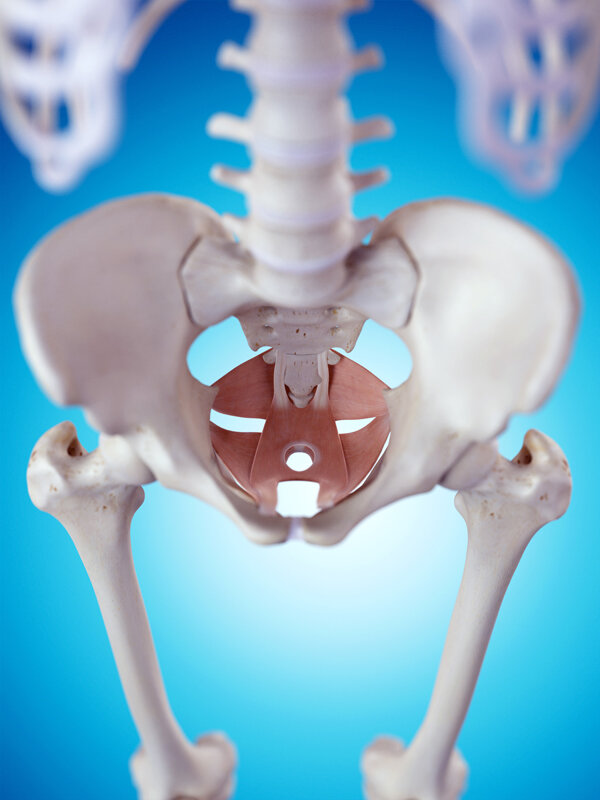
Vaginal birth and the risks of pelvic organ prolapse
/I was blowing up balloons for my daughter’s party the other day and felt I might be giving myself a pelvic organ prolapse! Pelvic organ prolapse is one of the most common health problems in Australia. 75% of women develop a pelvic organ prolapse during their lifetime! One in three will have a prolapse go to the entrance of the vagina or externally. Approximately 1 in 9 will have surgery for their prolapse however recurrence rates following surgery can be as high as 67% in the first year if there is co-existing pelvic floor muscle avulsion (ripping the muscle off the pubic bone)! (1). So surgery may not always be the best option. How can physiotherapy help?
“75% of women develop a pelvic organ prolapse in their lifetime!”
What is a pelvic organ prolapse?
The pelvic organs (the bladder, uterus, rectum and part of the small intestines) are supported in position by ligaments, the pelvic floor muscles and fascia. If the muscles weaken or the muscles and/ or fascia are torn (generally through vaginal child birth), the pelvic floor is weakened and doesn’t support the pelvic organs as well. Thus with this weakness, the organs can gradually drop down. Due to their position the organs fall to the centre, so the bladder falls backwards to push on the front wall of the vagina and the rectum pushes forwards to the back wall of the vagina and the uterus and small intestines move down into the vagina. Thus, a prolapse can be assessed via a vaginal examination by a Women’s Health Physiotherapist, Obstetrician, Gynaecologist or some GPs.
“a prolapse can be assessed via a vaginal examination by a Women’s Health Physiotherapist, Obstetrician, Gynaecologist or some GPs.”
What are the risk factors for getting a pelvic organ prolapse?
“The women most at risk of pelvic organ prolapse are... ones who have given birth”
The women most at risk of pelvic organ prolapse are ones with weakness or damage to the pelvic floor muscles, therefore any woman who has given birth, particularly those who have sustained an avulsion (1). During birth the levator ani (pelvic floor muscle) can stretch to 359% of its resting length! Skeletal muscle is meant to rupture once it has been stretched beyond 150% of its resting length (2). So birth can cause complete avulsion of the puborectalis and pubococcygeus muscles (levator ani). A study found 20% of women that had given birth to one baby had avulsion injuries! (2). Thus, avulsions and prolapse are a very real possibility and consideration for us giving birth vaginally.
“Avulsion is also more likely in those that have a forceps assisted delivery and those women that are older”
Another study found that women with an avulsion are two times as likely to get a pelvic organ prolapse, two times as likely to get a bladder prolapse (anterior vaginal wall prolapse) and four times as likely to get a uterine prolapse (3). Avulsion is also more likely in those that have a forceps assisted delivery and those women that are older. For women with two normal vaginal deliveries a 20 year old has 15% chance of avulsion compared to 40% for a 35 year old. For a woman who has had 2 children delivered by forceps risk of avulsion increases to 40% for a 20 year old and 80% for a 35 year old! (3). Vacuum assisted delivery or epidurals do not increase the risk. Other risks of avulsion are those with chronic respiratory conditions, chronic constipation, bulimia, regular heavy lifting or high impact elite athletes (gymnasts, runners) as these put regular increased pressure down on the pelvic floor.
“Other risks of avulsion are those with chronic respiratory conditions, chronic constipation, bulimia, regular heavy lifting or high impact elite athletes”
Signs of a pelvic organ prolapse
Signs of a prolapse is a heaviness or fullness in the vagina (as this is where the organs collapse to), lower abdomen pressure, low back pain, incomplete emptying on urination or defecation, needing to use the fingers to help defecate, recurrent UTIs, pain with sex, and when severe, a visible mass in or outside the vagina.
Can physiotherapy help my pelvic organ prolapse?
A Women’s Health Physiotherapist can help reduce or remove your prolapse by strengthening and coordinating your pelvic floor muscles (so that they come on when you need) and if the pelvic floor is too weak to support your activities you want to do (eg lifting your older children, running), vaginal support devices (pessaries) can be fitted in to the vagina to lift the organs back in to position.
Is there evidence that physiotherapy helps prolapse? Studies have shown that those women that had supervised pelvic muscle strength training with a physiotherapist significantly improved their prolapse symptoms and grade of prolapse compared to the control group who just received general advice on pelvic floor strengthening exercises (4). See the blogs Pregnancy, vaginal birth and stress urinary incontinence and Sax has cured my pelvic floor! and Pelvic floor strengthening and stretching- my story for tips on pelvic floor strengthening. However, as the research shows, you really need the hands on guidance of a women’s health physiotherapist to get the best results.
“Studies have shown that women that had supervised pelvic muscle strength training significantly improved their prolapse symptoms and grade of prolapse…”
Will a strong pelvic floor cure my prolapse?
Strengthening your pelvic floor has been shown to give significant lift to the pelvic floor organs (5). However, there will be some women where no amount of pelvic floor strengthening will reduce the prolapse. These will be with the cases with the higher grade prolapses where the fascia has been significantly damaged or the pelvic floor muscles have torn off the bone (avulsion).
“some women where no amount of pelvic floor strengthening will reduce the prolapse.”
In these cases, the best treatment is going to be the use of a pessary or pelvic floor organ prolapse surgery. A women’s health physiotherapist or gynaecologist will be able to assess which treatment will be the best for you. Pessaries can be just as effective as surgery so a good non-invasive option. Pessaries can be fitted by your specially trained GP, gynaecologist or physiotherapist.
“Pessaries can be just as effective as surgery so a good non-invasive option”
Will using a pessary strengthen my fascia and prevent or fix pelvic organ prolapse?
Quite possibly! After delivering your baby vaginally it is possible and important to reduce the stretch to your pelvic floor fascia and muscles. If done early, this can go a long way to preventing a or fixing a pelvic organ prolapse. This is because you can shorten and tighten the pelvic floor fascia/ collagen “scaffolding” to hold all the organs in place early after birth but not later.
While you are breastfeeding, you have significantly decreased oestrogen. This allows the shortening of the stretched pelvic floor fascia. After stopping breast feeding this potential markedly decreases.
Some studies have shown that, along with a quick return to your pelvic floor muscle strengthening exercises after birth, a pessary can lift and hold the fascia in a shortened position while it knits and heals. in a permanently shortened position (5).
“While you are breastfeeding, you have significantly decreased oestrogen. This allows the shortening of the stretched pelvic floor fascia. After stopping breast feeding this potential markedly decreases.”
How can I change my lifestyle to prevent or reduce a prolapse?
To reduce the strain down through the fascia, physiotherapists can look at your lifestyle etc and give advice on what might be putting pressure on the fascia. For example constipation, high body weight, respiratory conditions, heavy lifting and certain exercises are important to avoid or manage pelvic organ prolapses. Talk to your Women’s health physiotherapist about what exercises to avoid. If you do have a prolapse we can also give advice on how best to go to the toilet to complete emptying and suggest positions to make sex less painful.
Prolapses tend to worsen during the day as they gradually drop down with gravity. This can be counteracted though by contracting the pelvic floor upwards, especially in times of increased abdominal pressure, such as sneezing, coughing and jumping. Lying down with your legs and pelvis elevated for 10-20 minutes during the day (such as when your baby is sleeping) can help reduce the prolapse as well.
Surgery for POP
There are many different types of surgeries available for pelvic organ prolapses. In the most basic terms, surgeries can use sutures (stitching) or mesh tape to lift the “falling” organs such as the uterus, vagina, bladder and rectum. If there is a bladder (anterior) or rectum (posterior) prolapse the vaginal wall and underlying fascia can be sutured/ tightened to reduce the bladder/ rectum prolapse.
Unfortunately there is a poor success rate with the anterior prolapse suturing surgery (50-60%) so this is why mesh was introduced with better success rates. However, many of you would have heard of the controversy of mesh used for POP repairs. It has been found to potentially cause significant side effects including: infection, vaginal erosion, pain with sexual intercourse (dyspareunia), repeat prolapse, incontinence, pain when patients move and cutting the penis on intercourse. It must be highlighted that it is only one type of surgery using mesh (transvaginal mesh surgery) that has caused these significant effects. Mesh used to lift the vagina has much less rates of detrimental side effects and is still permitted to be used.
Several studies have shown that objectively (on assessment) that the mesh surgeries were more successful in preventing a recurrence of the prolapse than a suture repair. However, the studies also consistently showed that subjectively (the patient’s feeling about a potential prolapse) was the same for both surgeries (6). So with the risks of transvaginal mesh surgery, perhaps the suturing surgery is the better option for anterior (bladder) prolapse repairs? This is such a brief summary of the potential surgeries so please consult your Gynaecologist or Obstetrian for more information on your options.
Summary
Pelvic organ prolapse is very common in women especially those that have had vaginally birthed, had forceps delivery, are older mothers, have chronic respiratory conditions or constipation, bulimia, are regular heavy lifters or are high impact athletes.
Signs of prolapse are a heaviness or fullness in the vagina, low back pain, incomplete emptying on urination or defecation, recurrent UTIs, pain with sex or a visible bulge in or out of the vagina.
Women’s Health Physiotherapists have many ways to help you if you have a prolapse including pelvic floor strengthening, advice and pessary fitting.
References
Brown et al 2002, Pelvic organ prolapse surgery in the United States, AM J Obstetr Gynecol, (186) pp 712-716.
Ashton-Miller JA, Delancey JOL. 2009. On the Biomechanics of Vaginal Birth and Common Sequelae Annu Rev Biomed Eng 11: 163–176.
Dietz H, Simpson J. Levator trauma is associated with pelvic organ prolapse. BJOG 2008;115:979–984.
Stüpp, L., Resende, A.P.M., Oliveira, E. et al, 2011, Pelvic floor muscle training for treatment of pelvic organ prolapse: an assessor-blinded randomized controlled trial. Int Urogynecol J 22, 1233.
Braekken et al 2010, Morphological changes after PFMT measured by 3D ultrasounography, Am H of O and G.
Rudnick et al 2015, A 3 year follow up after anterior Colporrhaphy compared with collagen-coated transvaginal mesh for anterior vaginal wall prolapse: a randomised controlled trial, BJOG, vol 123 (1), pp 136-142.
Acknowledgement
I would like to acknowledge Taryn Hallam, director of the Women’ s Health Training Associates (WHTA) and the outstanding physiotherapist professional development courses she teaches. Her advanced course on stress urinary incontinence and pelvic organ prolapse is extensively researched and has provided much of the material for this blog. I can not recommend her courses highly enough.
Melli Tilbrook is the Physiotherapist and Director of Mummyotherapy and also works at Milkwood Studios, Tusmore